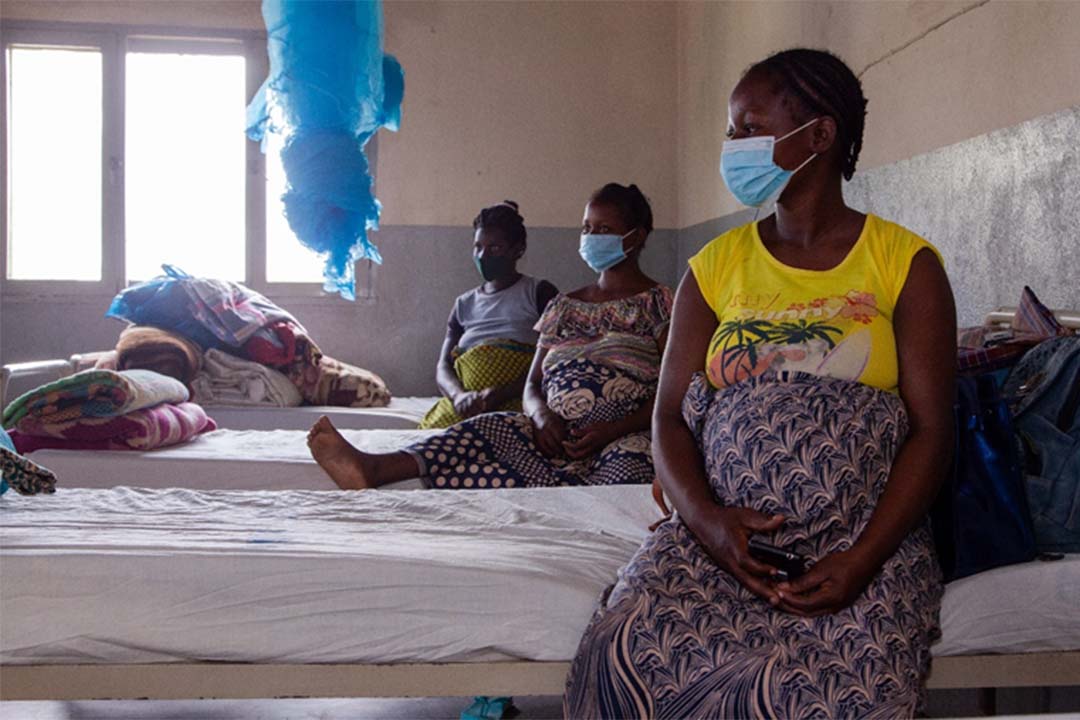
Delivering success: USask research sheds light on what makes maternity waiting homes work in low-income countries
Pregnancy- or childbirth-related death is rare in high-income, western countries, but not so in low- and middle-income countries.
The World Health Organization estimates there were about 300,000 maternal deaths globally in 2017—more than 800 women every day—with a vast majority of these deaths (nearly 85 per cent) occurring in Sub-Saharan Africa and Southern Asia.
To address the high number of maternal deaths, maternity waiting homes (MWHs) are built for women in low-and middle-income countries. Women about to deliver stay and access timely, professional care before, during, and after delivery. These MWHs can make a real difference for women who are at risk for complications or who live far from the nearest medical facility, in areas where motorized transport is scarce, and roads are not always easy to travel.
New research published by Dr. Nazeem Muhajarine (PhD) from the University of Saskatchewan’s (USask) College of Medicine, is tackling the unanswered questions of why, how, and under what conditions MWHs are successfully implemented so that they lead to the desired positive outcomes, namely, a safe delivery and mother and newborn returning home.
“Previous research has returned mixed findings, some showing maternity waiting homes had positive effects, with others showing no effect. None had investigated not only whether, but how and why and under what conditions the maternity waiting homes have the impact that they do,” said Muhajarine. “Our research addressed this complex question.”
Existing studies have addressed narrow aspects of whether MWHs work. Through a focused review and synthesis of more than 100 studies – from Africa, South America and Asia that used different data and methods, and were published in English, French, Spanish and Portuguese – Muhajarine’s team created nine sets of explanations about how and why MWHs succeed or fail to link women to a facility with skilled birth attendants. These findings were then validated through interviews conducted with 12 experts from five African countries who were knowledgeable about implementation of MWHs.
The research findings show that MWHs are successful when they meaningfully reach three groups – health-care providers and implementers, communities, and pregnant women and their families. An MWH is more likely to be successful where it is jointly owned and regulated by a government authority and the community it serves, with both levels contributing resources to develop, manage, and sustain good quality, user-centred services. These homes also need champions within the health system who believe and trust in the intervention, as well as health providers who are trained and sensitized to respectful and humanized care.
At the community level, influential local leaders must be involved in managing MWHs and mobilizing community members’ support. This helps to normalize use of MWHs and facility birth services in the community and builds a sense of collective ownership.
At the user level, joint efforts need to be made by governments and community leaders to educate and engage pregnant women and their families, especially the male partners and other close family members. Addressing concerns about use, creating a more homelike environment, and including activities that benefit women who are waiting to give birth, generates more demand for MWHs.
Muhajarine said this work has illuminated specific actions that need to be taken by government, health systems, communities, and pregnant women and their families for the successful uptake and sustainability of MWHs.
The USask team has established a long-lasting partnership in Mozambique, the Mozambique-Canada Maternal Health Project. The Provincial Health Directorate in Inhambane, and the Mozambique Project team led by Horacio Mandevo Chissaque are key partners in this research, and are the primary intended users.
The next step in this work is to test the team’s explanatory themes regarding MWH uptake and scale up in an evaluation of five MWHs built by the project with funding from Global Affairs Canada. The evaluation will identify what specific actions need to be taken to ensure that new and continuing MWH optimally serve mothers and their communities.

